Untersuchungen
1. Schwangerschaftsdrittel
Ultraschalldiagnostik
(11+0 – 13+6 Schwangerschaftswoche)
Die Ersttrimester-Diagnostik ist eine umfassende Untersuchung, die nach ausführlicher Aufklärung – angepasst an Ihre individuellen Bedürfnisse – mehrere Bestandteile beinhalten kann:
- Beurteilung der körperlichen Entwicklung des Fetus (qualifizierte Feinultraschalluntersuchung / früher Fehlbildungsausschluss)
- Berechnung des Risikos für Chromosomenstörungen (Nackentransparenzmessung mit Bestimmung der Plazentahormone ß-HCG und PAPP -A)
- Berechnung des Risikos für eine Schwangerschaftsvergiftung (Präeklampsie-Screening mit Bestimmung des Placenta Growth Factor PlGF)
- Cell-free DNA Test (Nicht invasiver Pränatal-Test NIPT)
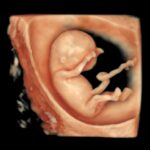
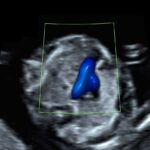
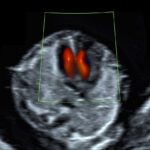
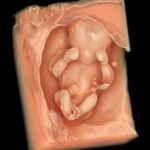
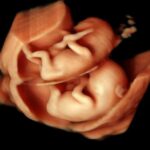
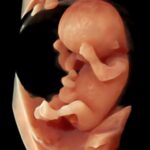
Zum ersten Mal in der Schwangerschaft ist eine Untersuchung des ganzen Kindes im Detail möglich. Bereits im I. Schwangerschaftsdrittel können viele schwere Fehlbildungen – insbesondere des Kopfes und des Gehirns, der Arme und Beine, Spaltbildungen der Bauchwand und Wirbelsäule, Zwerchfelldefekte und der Harnblase entdeckt oder weitgehend ausgeschlossen werden. Des Weiteren kann bereits ein Teil der schweren Herzfehler durch einen frühzeitigen Herzultraschall (frühe fetale Echokardiographie) erkannt werden. Damit können Risikosituationen bereits früh erkannt und einem optimalen Management zugeführt werden.
Daher ist diese detaillierte frühe Ultraschalluntersuchung immer ein wichtiger Bestandteil der Ersttrimester-Diagnostik.
Im Anschluss an eine unauffällige Ultraschalluntersuchung gibt es drei weitere Vorgehensweisen: entweder basiert die Risikoberechnung für die Trisomien 13, 18 und 21 auf der gemessenen Nackenfaltenmessung allein oder ergänzt durch eine Blutabnahme der Plazentahormone ß-HCG und PAPP-A (klassisches Ersttrimesterscreening). Diese Risikoberechnung wird inzwischen jedoch oftmals durch den Nicht-invasiven Pränatal-Test ersetzt, der entweder bereits im Vorfeld zu unserer Untersuchung durch Ihren Frauenarzt abgenommen wurde oder im Anschluss an die Ultraschalluntersuchung auch bei uns erfolgen kann.
Berechnung des Risikos für Chromosomenstörungen (Nackentransparenzmessung ggf. mit Bestimmung der Plazentahormone ß-HCG und PAPP -A)
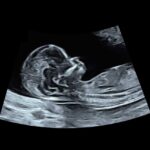
Der Begriff NT (Nackentransparenz, engl. Nuchal Translucency) beschreibt eine unter der Haut gelegene Flüssigkeitsansammlung zwischen Haut und Weichteilgewebe im Bereich des kindlichen Nackens. Mit der Messung der NT zwischen der 11+0 und 13+6 Schwangerschaftswoche (bzw. 45-84 mm SSL) soll beurteilt werden, ob ein statistisch erhöhtes Risiko vorliegt für ein Kind mit einer Trisomie 21 (Down-Syndrom), einer Trisomie 18 (Edwards-Syndrom) bzw. einer Trisomie 13 (Pätau-Syndrom). Führt man in allen Fällen mit einer NT oberhalb der 95. Perzentile eine Chromosomenanalyse durch, werden rund 75% der Schwangerschaften mit einer Trisomie erkannt. Eine differenziertere Risikoanalyse unter Berücksichtigung von Alter und Vorgeschichte kann die Erkennungsrate auf über 80% erhöhen. In Kombination mit zwei biochemischen Laborwerten (PAPP-A und freies ß-hCG) im mütterlichen Blut wird die Entdeckungsrate nochmals um 10% auf 90% erhöht.
Sollte sich ein erhöhtes Risiko ergeben, so werden wir zusammen mit Ihnen besprechen, ob und in welcher Form eine weiterführende nicht-invasive (vgl. NIPT) oder ggf. invasive Diagnostik (Amniozentese, Chorionzottenbiopsie) erfolgen soll. In dieser Beratungssituation gehen wir dabei immer auf Ihre individuellen Vorstellungen und Wünsche ein.
Eine verbreiterte NT findet sich überdurchschnittlich häufig auch bei Kindern mit einem Herzfehler oder einer Vielzahl anderer, in der Literatur beschriebener Erkrankungen (z.B. Skelettauffälligkeiten und Stoffwechselstörungen), so dass bei unauffälliger Chromosomenanalyse eine frühe Organdiagnostik (Feinultraschall) und detaillierte Untersuchung des Herzens (fetale Echokardiografie) veranlasst werden können
Die erforderliche Software-Lizenz für die Risikoanalyse wird nur den Untersuchern zur Verfügung gestellt, die von der Fetal Medicine Foundation London zertifiziert wurden. Anhand des dadurch ermittelten Risikoprofils kann die Entscheidung hinsichtlich einer weiterführenden Diagnostik (z.B. NIPT, Feinultraschall, Chorionzottenbiopsie, Amniozentese) individualisiert werden.
Berechnung des Risikos für eine Schwangerschaftsvergiftung (Präeklampsie-Screening mit Bestimmung des Placenta Growth Factor PlGF)
Die Präeklampsie (sog. Schwangerschaftsvergiftung) und Plazentaunterfunktion sind weitere Risikosituationen, die im Rahmen der Ersttrimester-Diagnostik in unserer Praxis eingeschätzt werden. Hierzu kann am Tag der Ultraschalluntersuchung zusätzlich zu Gewichts- und Blutdruckmessungen der Biomarker PlGF abgenommen werden. Bei erhöhtem Risiko kann prophylaktisch / therapeutisch eingegriffen und durch eine geeignete Überwachung der Schwangerschaft zu einer Verbesserung des Schwangerschaftsverlaufes beigetragen werden.
Cell-free DNA Test (Nicht invasiver Pränatal-Test NIPT)
Beim NIPT wird Ihnen Blut zur Bestimmung der zellfreien DNA im mütterlichen Blut abgenommen. Mit diesem Screening-Verfahren werden etwa 99% der Feten mit Trisomie 21 erkannt bei einem niedrigen falsch-positiven Ergebnis (etwa 0,1%). In etwa 2-3% der Fälle bleibt die zellfreie DNA-Analyse ohne Ergebnis und kann wiederholt werden. Wenn erneut kein Ergebnis erzielt werden kann, sollte eine Fruchtwasser- oder Mutterkuchenpunktion erfolgen, da das Risiko für eine Chromosomenstörung bei Testversagen ansteigt.
Der seit 2012 verfügbare Test auf Trisomie 21, 13 und 18 (vgl. NIPT) aus dem mütterlichen Blut, der seit 01.07.2022 bei Indikation auch von den Krankenkassen bezahlt wird, kann die Ersttrimester-Diagnostik nicht ersetzen, da er keine Aussage über andere Chromosomenstörungen, genetische Erkrankungen oder Fehlbildungen des Fetus treffen kann. In bestimmten Situationen kann er als Ergänzung des Ersttrimester-Screenings sinnvoll sein. Die deutsche Gesellschaft für Ultraschall in der Medizin e.v. hat 10 goldene Regeln für die Durchführung eines NIPT-Tests veröffentlicht (10 goldene Regeln NIPT). Noch mehr Sicherheit erreichen Sie, wenn Sie eine Chromosomenanalyse vornehmen lassen (Amniozentese, Chorionzottenbiopsie). Hierzu beraten wir Sie im Rahmen der Ersttrimester-Diagnostik bei uns.
Sollte bereits vor der sonografischen Ersttrimester-Diagnostik ein nicht-invasiver DNA-Test mit unauffälligem Ergebnis vorliegen, so wird auf die Risikoberechnung für die Trisomien sowie meist auch auf die Bestimmung der Plazentahormone ß-HCG und PAPP-A verzichtet.